The Three Ways PBMs Make Money: Rebates, Admin Fees and Spread
When working with a Pharmacy Benefit Manager (PBM), it is important to understand exactly how they extract profits. They act as the middleman between the pharmaceutical industry and employers, promising lower costs and a streamlined health care process. So, what’s in it for them? – Quite a lot, as they hold the power of prescription drug costs for employers.
Traditional PBMs make a profit by obtaining money in 3 key categories: rebates, admin fees and spread.
How PBMs Make Money
All PBMs will tell you they want to optimize your pharmacy benefit program, but without transparent values and public benefit at their core, many traditional PBMs may have a different goal in mind. For example, traditional PBMs often avoid generic medications in order to benefit from expensive brand-name pharmaceuticals. To understand your PBM’s contract language when discussing your plan, read on. This could help you save money on health care costs by negotiating and better understanding your contract agreement.
Rebates
A rebate is a discount on the medication that a drug manufacturer gives a PBM in return for agreeing to offer their pharmaceutical drug or product on a formulary list for an employer’s pharmacy benefit plan. Traditional PBMs commonly push the narrative that employers receive “100% of rebates” when only a portion of rebates are shared with the self-insured employer. Your PBM typically pockets the rest.
If a PBM states the employer receives “100% of rebates,” this should raise a red flag. Contract language has become so sophisticated that even a few years ago if a pharmacy paid a PBM $500, they would call $450 rebates and $50 other fees. Today, they may call only $300 of the $500 rebates. With the additional fees listed below, they can drastically improve their profits while at the same time continuing this positive narrative to employers by telling them they get 100% of the rebates. Although that is accurate, employers are still losing out.
So, while the net manufacturer prices—the cost of medicines after all discounts and rebates have been paid—have been following a declining trend over the last five years, these discounts are offered to wholesalers and pharmacies, not necessarily lowering the cost of prescriptions for members.
Rebates may show as “included” on your PBM contract agreement, but many additional profit sources need to be reviewed. To understand these as an employer, ask your PBM to disclose all sources of pharma funding in the contract between pharma and the PBM. If they don’t – ask more questions!
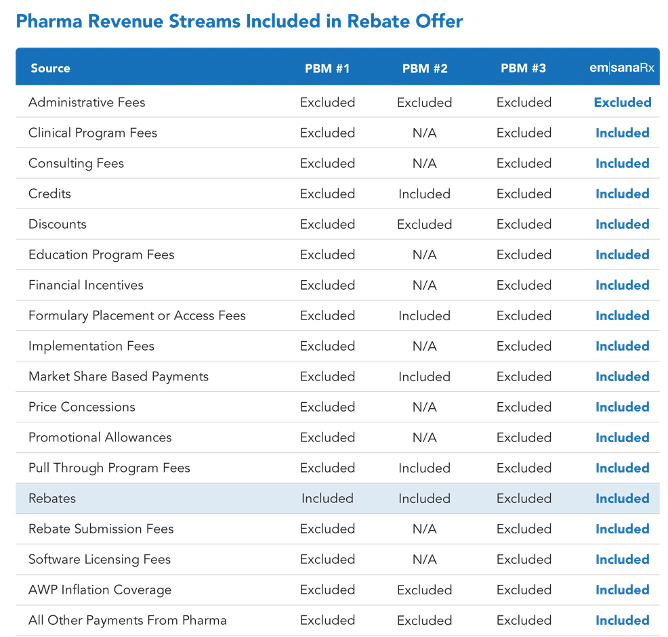
Admin Fees
Administrative fees are fees and payments that the PBM keeps for themselves – the cost of doing business. These fees are factored into the cost of working with a PBM and offer little to no transparency regarding how they are added to the employers’ contracts. Even the savviest of employers cannot typically understand the various charges they are paying due to complex drug contracting.
These fees also drive up the cost of drugs, requiring an even more significant percentage of total drug costs to go towards a PBM’s profit, and when these costs go up, they direct impact plan members who are likely in a high deductible health plan.
Spread
Further, PBMs make money through a term called “spread.” This is the practice of reimbursing the pharmacy one amount for a medication and charging the employer or plan sponsor a higher price for the same drug. What does the PBM do with the difference? They pocket it.
Although some PBMs say they have eliminated “spread,” employers must keep an eye out because although spread may be eliminated, there are PBMs starting to pay their own pharmacies more than other pharmacies to keep that money flowing within their network.
PBMs have many ways of extracting profits without an employer’s notice. These tactics are commonly hidden in contracts by way of complex industry wording and definitions.
The More You Know
Understanding the intricate details of pharmacy benefit managers and the way they structure their programs will help employers negotiate better contracts for an optimized health plan. The pharmaceutical industry is riddled with money-hungry tactics and employers need to be wary of these details to protect their members.
Do your research – only a select few companies truly work with their clients to provide low-cost, high-quality pharmacy benefit plans. Traditional, for-profit PBMs make money their sole focus, but AffirmedRx changed our corporation status to a Public Benefit Corporation for good reason. We have a completely employer-focused and member-focused model, eliminating all additional layers so there are no hidden fees. This means that our main priority is to help the public gain access to their pharmacy benefits without being gouged by the prices. We focus on the people, not the profit.
